A media association, they say, is as good as its members.
For an association to prosper and keep on soaring, it must listen to the changing needs of her
members. And so, when members of our association, the Media for Environment, Science,
Health and Agriculture (MESHA), requested, through our very active members only WhatsApp
group for a training on mobile journalism (MOJO) last December, the leadership led by our
Secretary, Aghan Daniel, listened.
“We have to keep on with the demands of a dynamic and ever evolving media landscape, print,
online and radio lest our association becomes a dinosaur,” said Aghan during the opening of the
training held from March 31- April 1, 2022.
The training targeted journalists with a revolutionary approach to telling science stories in
keeping with a fast paced world.
Members, 15 of them, were introduced to the MOJO concept and its elements. Trainees heard
that MOJO is an all around multimedia solo reporting act in which the smartphone serves as a
complete production unit for collecting, editing and disseminating news.

Emmanuel Yegon, a multi-media journalist unpacked MOJO as the most critical tool for
journalists as it helps transcend many challenges facing journalists.
Yegon trained through a highly interactive classroom setting that included lectures, question and
answer sessions as well as practical assignments. He first unpacked MOJO as a form of digital
storytelling where a smartphone is used to collect or create data in audio, images and videos.
The smartphone is further used to edit collected or created content and to disseminate content. As
a full production unit, there is no limit on how far one can go to collect news, features and
relevant information.
He trained journalists on what he termed as a “new workflow for media storytelling where
reporters are trained and equipped for being fully autonomous.”
The first day of training was anchored on two key factors. First, that MOJO enables reporters to
undertake multiple production and content distribution activities using one single device.
Second, the audience have access to the same means of producing content allowing for them to
similarly consume content through mobile devices. As such, MOJO is a cross-platform and
digital innovation approach within the reach of reporters in far flung areas.
Participants discussed storyboarding, or story planning using mobile devices. They were also
taken through elements of a practical MOJO toolkit which includes a quality smartphone, a
microphone, a simple LED light, a power bank and tripod.
The trainees were also taken through the dos and don’ts of MOJO including not zooming while
recording images or collecting videos. Reporters were further taken through tips in image
orientation and direction. They were advised not to mix both landscape and portrait images while
creating content.
The viability of taking photos, videos, audio and graphics, editing and uploading to their
respective newsroom servers were also discussed. The trainer encouraged reporters to own or
have access to a smartphone and to develop skills on MOJO as this is the new frontier of content
creation, production and dissemination.
MOJO, in essence, participants heard, is a solo media production unit. Practical sessions
included how a lone journalist can use a single mobile devise to tell their story, from breaking
news, news features to more timeless human interest stories.
Reporters saw firsthand how they can achieve the greatest value from their smart phones as a
production studio in their pockets. This form of reporting is a cost effective platform, portable
and convenient.
For investigative reporters, it is a safe platform to discreetly collect information without
detection. By the same token, MOJO can help a journalist to stay safe when recording sensitive
information.
MOJO is also flexible and a journalist can produce content at a faster pace. Reporters were also
taken through video recording apps or camera apps that can help them capture quality images.
By further connecting their smartphone to an external microphone, they can record quality
sound. This, Yegon says, is akin to putting an entire production unit in the pocket. More
importantly, an entire newsroom can put these simple device production units in the hands of
more journalists.
“Those lessons were the most interesting thing I had been through in the recent past,” said Rachel
Kibui from Nakuru. Her counterpart from Kitui, in Eastern Kenya, Nzengu Musembi added that
“the sessions were pretty educative. From this training, I can see myself being a competent
mobile journalist.”
By Joyce Chimbi


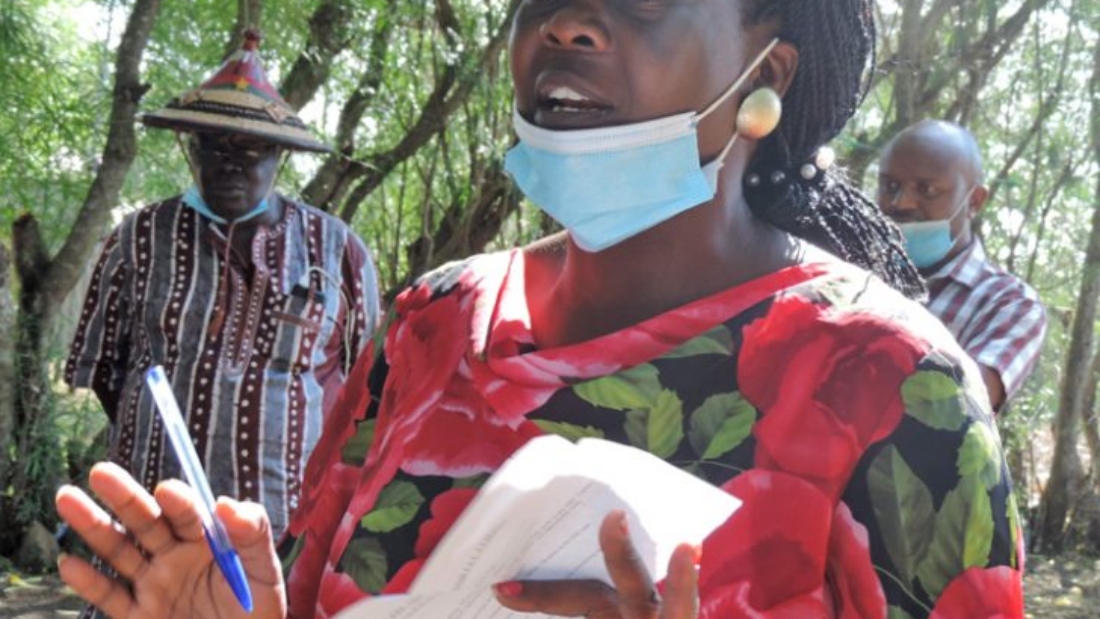

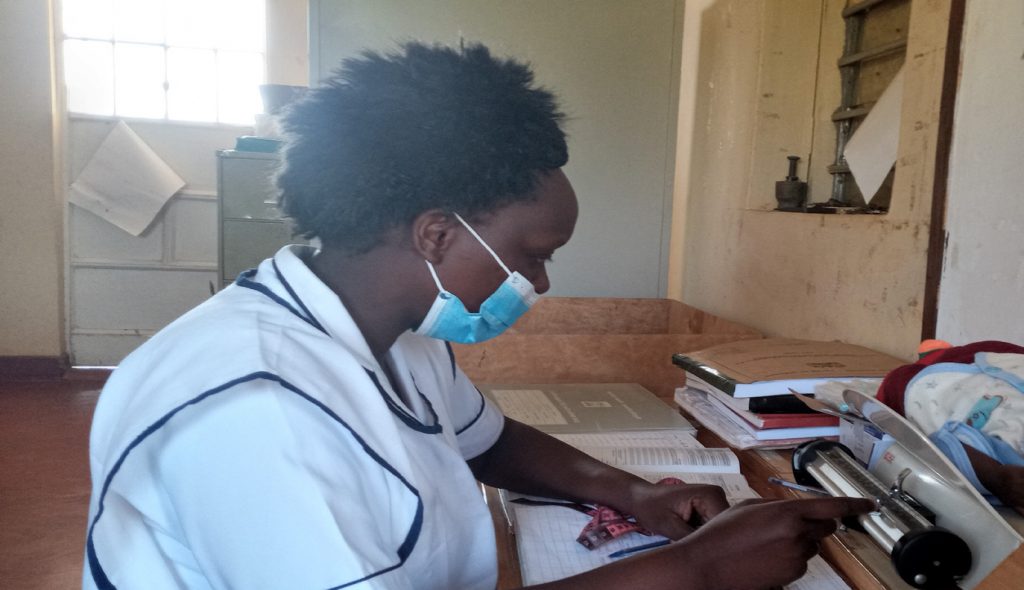 Anita Nyambura, a consultant laboratory technician with a private hospital in Nakuru County, states that telemedicine is the provision of health services, in this case for people living with HIV through a wide range of platform such as video, phone calls, social media and mobile phone apps designed for this very purposes.
Anita Nyambura, a consultant laboratory technician with a private hospital in Nakuru County, states that telemedicine is the provision of health services, in this case for people living with HIV through a wide range of platform such as video, phone calls, social media and mobile phone apps designed for this very purposes.
 vaccine in South Africa and that here in Kenya, they at KAVI in collaboration with partners in USA and Canada are working on Antibody Mediated Prevention (AMP) study and HVTN 706, also known as Mosaic.
vaccine in South Africa and that here in Kenya, they at KAVI in collaboration with partners in USA and Canada are working on Antibody Mediated Prevention (AMP) study and HVTN 706, also known as Mosaic.

 People living with HIV are no longer as sickly as they used to be. It is therefore now possible for a HIV positive individual with a very high viral load and therefore highly infectious to appear healthy.
People living with HIV are no longer as sickly as they used to be. It is therefore now possible for a HIV positive individual with a very high viral load and therefore highly infectious to appear healthy.
 What about the study on vaccines and drugs?
What about the study on vaccines and drugs?