By Chemtai Kirui | phillykirui@gmail.com
Journalists have been urged to strengthen accuracy in post-pandemic reporting by relying on credible sources and contribute to a better-informed public.
The call was made during a media science café held in Nairobi on February 9, 2024. The café, which was training of journalists on health reporting with a focus on pandemic preparedness, was organised by the Media for Environment, Science, Health, and Agriculture (MESHA).

John Muchangi, the Science Editor at the Star newspaper, said that there is still a lot of unexplored information on pandemics and epidemics, which can significantly increase public awareness.
“In my experience, reporting on a pandemic is a marathon without an end,” said Muchangi, who reported his continued coverage of COVID-19 with over 300 articles to his name so far.
He said that just because the World Health Organisation (WHO) declared the end of COVID-19 as an international public health emergency, it does not mean that there are no stories that journalists can tell today on health concerns and other developments in pandemics or epidemics.
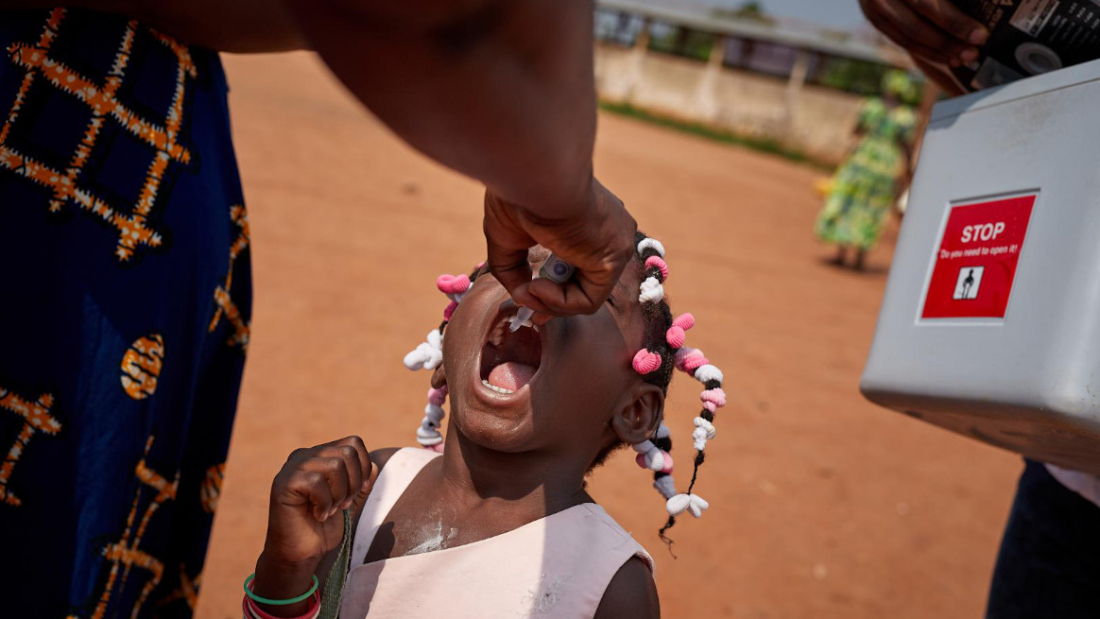
“People still need a vaccine, don’t they? Let’s look at malaria. The only vaccine available for malaria in Kenya now has an efficacy of about 36%. Does that mean that people should opt out because the efficacy is low?” he posed.
“If that is the only option, people will go for it, and that is where journalism comes in – letting the public know about this vaccine, where it is provided from, and how much it costs.”
Muchangi, however, urged journalists reporting on these scientific topics to check their ego and always be willing to be corrected where necessary.
“I once wrote a story where I compared one malaria vaccine with another, and reported that one vaccine worked better than the other based on the information I had at the moment,” he recalled.
“When the story was published, I got a lot of emails from concerned bodies such as the World Health Organisation, saying that the reporting was inaccurate.”
Muchangi said that the experience was disheartening since many journalists do not want to be questioned on their work, but after a lot of conversation, he realised that he had given the comparison of the vaccine based on differentiated variables and accepted his shortcomings.

To avoid such scenarios, Muchangi recommended that journalists stay vigilant in the dynamic landscape of science and conduct research from reliable reports such as from the Kenya Demographic and Health Survey (KDHS).
Among the attendees of the media science café was Audry Awino, an 18-year-old journalism student and host at Maseno University’s radio station, Maseno Radio. She said the training motivated her to actively seek out untold stories that have yet to capture public attention.
“When Muchangi said that in the last 50 weeks, no COVID-19 cases in Kenya have been reported in the WHO database, yet Kiambu County recently reported three cases, it showed that there is a gap that needs to be addressed,” Awino said.
Godfrey Ombogo, the immediate former editor at Sayansi Magazine and a member of MESHA, delivered a presentation on writing an impactful health story.
He said that a compelling health report should be supported by credible and relevant data, as numbers play a crucial role in conveying science stories to the audience.

“When writing for Sayansi Magazine, one should have multiple sources, at a minimum three,” Ombogo said. “The sources, including experts, government agencies and beneficiaries, will provide a comprehensive and well-rounded perspective of the story you are reporting on.”
Ombogo further encouraged the use of data from reputable sources such as WHO and United Nations, surveys, studies, and local authorities to strengthen the credibility and impact of health stories.